Rapid Systematic Review Age-adjusted D-dimer for Ruling Out Pulmonary Embolism
Original Commodity
D-dimer value in the diagnosis of pulmonary embolism—may information technology exclude only?
Introduction
PE ordinarily results from an occlusion of the pulmonary artery or its branches by a thromboembolus (1). PE is usually ane of clinical manifestations of venous thromboembolism disease (VTE) and is the third (later ischemic heart affliction and cerebrovascular illness) most frequent cardiovascular disease with an incidence of 1–2% in the general population and 12–twenty% among hospitalized patients (2-4). Approximately 60% of all VTE cases are found in hospitalized patients. Among those, 5–10% suffer from PE (2,5,six). Clinicians are concerned about PE, because of its high gamble of mortality (7-10).
If left untreated (about oftentimes because undiagnosed), acute PE has a lethality high as 59%, whereas adequately treated acute PE leads to decease in only seven% of cases (xi). The gilded standard for the diagnosis of PE is computed tomographic pulmonary angiography (CTPA) (12). However, CTPA has sure disadvantages such as radiation exposure, the need for contrast medium administration, which may crusade renal failure and the high cost of the test (13). Therefore, less invasive and less expensive diagnostic tools are desirable. One of currently unresolved question is whether plasma D-dimer assays may be considered as reliable test both for excluding PE and for screening for patients at the highest risk. Plasma D-dimers are cross-linked fibrin derivatives produced when fibrin is degraded past plasmin. Elevated D-dimer levels are found in many atmospheric condition that lead to activation of blood coagulation and fibrin formation (14). Since the 1980'south. researchers take been trying to create algorithms useful for ruling out PE with plasma D-dimer assays (15-26). In almost all trials the cutoff betoken was established at the level of 500 ng/mL, but it was helpful only to rule out PE in patients with depression and moderate clinical probability of PE. Thereafter plasma D-dimer assays accept been studied in various aspects connected with VTE: the correlation of D-dimer levels with brusk-term or long-term mortality (27), the severity of the grade of the disease (28), predicting disease relapse afterward stopping anticoagulant therapy (29), and correlation with radiological severity of PE (30). In addition, 2 studies reported the presence of correlation between increased D-dimer levels and the likelihood of PE diagnosis by CTPA (31,32). The aim of our study is to determine the practical plasma D-dimer level above which the risk of PE is sufficiently high that CTPA is mandatory.
Methods
Report population and data acquisition
We retrospectively analyzed medical history notes of patients at University Teaching Hospital (SP CSK im. Kornela Gibińskiego in Katowice, Poland). In the hospital database from January 2009 through December 2013 we selected all patients with both a D-dimer blood level test and CTPA performed. Our inclusion criteria fulfilled 370 patients from nine wards of the hospital (Table i). Nosotros then divided the sample into two groups: patients with PE confirmed past CTPA and those without such a diagnosis.
Plasma D-dimer analysis
Plasma D-dimer levels were measured used automated quantitative latex-based, immuno-agglutination assay (HemosIL D-Dimer HS 500) (33). We included D-dimer results obtained inside 48 hours before CTPA was performed. Positive test effect was defined equally a D-dimer level of >500 ng/mL. A normal D-dimer range was defined every bit <500 ng/mL.
CTPA
PE had been diagnosed past CTPA in the presence of filling defects in pulmonary arteries or images suggesting pulmonary microembolism interpreted by certified experienced radiologists.
Statistical analysis
Analysis was performed using Statistica (http://www.statistica.com/) software version 10. Receiver operating characteristic (ROC) curve were built to make up one's mind the best cutoff value for the diagnosis of PE. We beginning included all records and 2d excluded patients from surgical wards. In addition, ROC curves were built for patients aged >65 and ≤65 with and without the history of tumour according to the most important risk factors of thromboembolism. Because of the retrospective pattern of the study important clinical characteristics such as tumour blazon were not recorded. Youden'due south index was calculated (YI = sensitivity + specificity – i) for each coordinate bespeak of the ROC curve to determine the cut-off value with the maximum sensitivity and specificity.
Results
The written report population included 189 men and 181 women. A full of 134 patients (36.two%) were diagnosed with PE and 236 patients (63.viii%) were negative for PE. The mean plasma D-dimer level in the group with confirmed PE (five,056 ng/mL) was significantly college than in the group of patients without PE diagnosis (2,920 ng/mL); P<0.05. The baseline characteristics of the written report population are shown in Table 1. The relative frequency PE diagnosis past D-dimer range is shown in Effigy i.
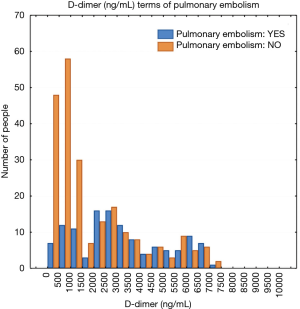
Figure one Relative frequency of PE diagnosis by D-dimer range (ng/mL). PE, pulmonary embolism.
Patients with positive D-dimer exam
The construction of the ROC curve immune u.s. to determine the best cut-off indicate. Having D-dimer values higher up 2,152 ng/mL significantly increased the likelihood of a PE diagnosis [surface area under curve (AUC) of 0.69; 95% CI, 0.64–0.74; P<0.05] (Figure 2). Edifice a second ROC curve excluding patients from surgical wards (surgery, gynecology, perinatology, intensive intendance unit) provided similar results (the best cutoff point was 2,152 ng/mL with an AUC of 0.71; 95% CI, 0.65–0.77; P<0.05).
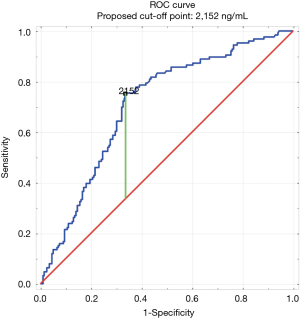
Figure 2 Receiver operating characteristic curve for PE diagnosis past D-dimer level (ng/mL). All patients included (north=370). PE, pulmonary embolism.
The sensitivity, specificity, PPV and negative predictive value (NPV) were calculated for different values of D-dimer concentration. For the best cutoff point (two,152 ng/mL) determined in this study, the specificity was increased from 20.3% to 62.vii% (in comparison to the results for the 500 ng/mL cutoff typically used), whereas its sensitivity was at 75.iv%. As well, the PPV was raised past xiii.1% (from forty.3% to 53.4%), while the NPV decreased only by v.6% (from 87.iii% to 81.8%).
The construction of another ROC curves immune us to make up one's mind the best cut-off points of D-dimer levels in 4 group samples divided according to the patients age (>65 or ≤65) years of age and the history of neoplasm. In our study, 96 patients (25.9%) had malignancy. Patients with the history of neoplasm and aged >65 had significantly increased likelihood of PE diagnosis at the D-dimer level of 2,652 ng/mL with an AUC of 0.67; 95% CI, 0.52–0.81; P<0.05 (Figure 3), whereas in patients aged ≤65 the best cut-off point was ii,563 ng/mL with an AUC of 0.69; 95% CI, 0.5–0.86; P=0.05 (Figure 4). Patients who did not suffer from neoplasm and were more 65 years former had D-dimer cutting-off signal adamant at the level of 2,169 ng/mL with an AUC of 0.71; 95% CI, 0.62–0.79; P<0.05 (Effigy 5), whereas in patients aged ≤65 the best cut-off betoken was 1,093 ng/mL with an AUC of 0.7; 95% CI, 0.61–0.79; P<0.05 (Figure 6).
We likewise assessed the accuracy of D-dimer test in excluding PE in patients with malignancy—sensitivity was 94.6%, specificity was 6.8%, PPV 38.ix% and NPV 66.seven%.
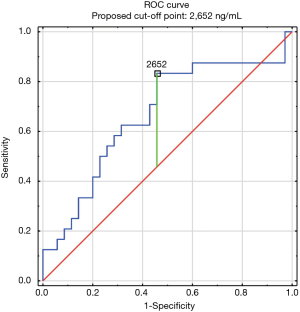
Figure 3 Receiver operating characteristic curve for PE diagnosis by D-dimer level (ng/mL). Patients with the history of tumour and anile >65 (northward=59). PE, pulmonary embolism.
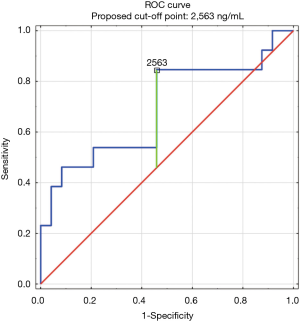
Figure 4 Receiver operating feature curve for PE diagnosis by D-dimer level (ng/mL). Patients with the history of tumour and aged ≤65 (northward=37). PE, pulmonary embolism.
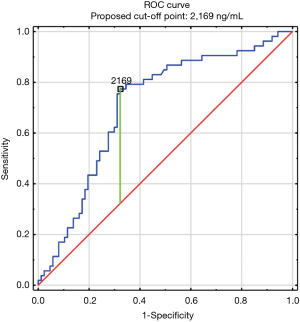
Effigy 5 Receiver operating characteristic curve for PE diagnosis by D-dimer level (ng/mL). Patients without the history of tumour and anile >65 (northward=140). PE, pulmonary embolism.
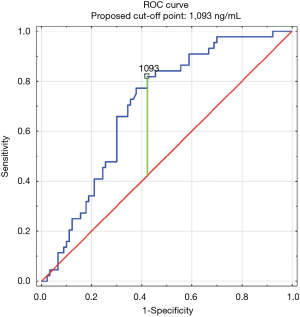
Figure 6 Receiver operating characteristic bend for PE diagnosis past D-dimer level (ng/mL). Patients without the history of tumour and aged ≤65 (n=134). PE, pulmonary embolism.
Patients with negative D-dimer test
In our study, 55 patients had negative D-dimer event (under 500 ng/mL) and seven (12.7%) of them had PE confirmed past CTPA, of which 2 (28.half dozen%) had subsegmental PE. We too checked why CTPA was performed despite normal D-dimer concentrations in these patients. Of the 55 patients, 48 (87.27%) had extended diagnostics because they had worrying clinical symptoms and/or PE adventure factors, two (3.six%) had pneumonia after ineffective grade of antibiotics, two (iii.vi%) had higher D-dimer exam levels before they were admitted to the infirmary, 2 (iii.6%) had CTPA performed to exclude other diseases (e.grand., vascular malformations) and i (i.8%) could not exist explained.
Word
The most important result of our report is the finding that highly elevated plasma D-dimer values (in our laboratory—2,152 ng/mL) are associated with significantly higher risk of PE. Our value of two,152 ng/mL is approximately four times higher than the normal plasma D-dimer cut-off value. This finding has aroused researchers' involvement in investigating the all-time D-dimer cut-off level for diagnostics of PE. I of the studies based on ROC curves, determined the all-time cutting-off level to be 830 ng/mL (AUC 0.762; 95% CI, 0.653–0.850; P<0.05), which is 1.5 times college than the normal D-dimer concentration for that laboratory (500 ng/mL) (34). In another study, the best cutting-off level based on ROC curve was determined to exist 900 ng/mL (AUC 0.76; 95% CI, 0.69–0.82; P<0.001), which also was 1.v times higher than the normal D-dimer value (580 ng/mL for that laboratory) (31). Analysis of the ROC bend in our report showed that patients with D-dimer values >2,152 ng/mL accept a 69% increased risk of developing PE. In comparison, the studies previously cited indicated that cutting-off levels of 830 ng/mL or 900 ng/mL have ~76% increased risk of developing PE (31,34). Even so, these studies had relatively pocket-sized study populations and only few patients with confirmed PE. The first study had simply 58 patients with PE (31) and the second had merely 40 (34), whereas in our report 134 patients had confirmed PE. In addition, we analyzed medical histories of patients from ix different wards of the infirmary, including internal medicine wards and surgical wards, whereas the previous studies analyzed merely patients from the department of internal diseases (34) and the emergency department (31). The data on specificity and sensitivity in our study are in keeping with the conclusions of a systematic review of the literature: more than sensitive is the assay less specific it becomes (35). There are large differences in proposed cut-off levels proposed for PE i,five times in the cited studies (31,33) which may result in a pregnant number of unnecessary CTPA. On the other manus, our results indicate that some patients with lower plasma D-dimer concentrations have acute PE. Therefore, prospective large calibration, multicenter study should be conducted to obtain the best cut-off level.
According to the latest [2014] guidelines on the diagnosis and management of acute pulmonary embolism (PE), the PPV of elevated D-dimer levels is low and D-dimer testing is not useful for confirmation of PE and elevated D-dimer concentration has prognostic value just for short-term bloodshed (36). Our findings bespeak otherwise. D-dimer levels may accept of import prognostic value in the diagnosis of PE therefore patients with depression clinical probability of PE and D-dimer concentration 4 times exceeding normal value should be assessed carefully and considered for CTPA.
It is well known that plasma D-dimer levels may be elevated past many clinical conditions, such as postoperatively and during pregnancy (37). Therefore, we decided to exclude such cases and examine but non-surgical patients. Past building some other ROC curve with the exclusion of surgical patients (Surgery, Gynecology, Perinatology, and ICU), we arrived at the same cut-off indicate (two,152 ng/mL), with an AUC of 0.7 which indicates a comparable risk of developing PE as found using the full sample. This is the proof that our cut-off point isn't overestimated because of other, D-dimers related conditions.
After analyzing other PE risk factors, we take determined whether the presence of two other of import adventure factors from Revised Geneva Score alter the cut-off points at which the likelihood of PE rises (12). Patients with an history of neoplasm had a significantly increased D-dimer cut-off level, than patients without such history regardless of their age. At the reverse, age was a significant factor in the patients without history of neoplasm with a significantly increased D-dimer cut-off level in patients >65 years former compared with those ≤65 years former. The historic period-adapted D-dimer cutting off bespeak is already a well-established method of ruling out PE (38), but we suggest that a amend fashion to determine the best cutting-off point above which significantly increases the likelihood of PE diagnosis is to accept the patients age as in Revised Geneva Score compared with using historic period-adjusted D-dimer cut-off levels. To the best of our knowledge our paper seems to exist the first to draw the likelihood of PE in such groups of patients. There were only reports well-nigh importance of those two take a chance factors in ruling out the PE, especially using age-adjusted D-dimer cut-off levels (39).
Moreover, it is worth to mention that in our study population at that place were 96 (25.nine%) patients with malignancy while in the Geneva score study (40) only 13% [138] of patients in their cohort had malignancy. Karamat et al. assessed the utility of D-dimer test in predicting PE in 104 cancer patients (41) and we had like sensitivity (94.half dozen% vs. 95.5%), lower specificity (half dozen.8% vs. 28.ii%), equally well as the PPV (38.9 vs. 42.8) and the NPV (66.7% vs. 91.6%) was lower.
It should also exist underlined that in our study a negative D-dimer test does not exclude the presence of astute PE 100% of the time, because 12.7% of the patients with normal plasma D-dimer levels had confirmed PE. Furthermore, among all patients with confirmed PE in our report, 7 of 134 (v.two%) had normal D-dimer concentrations. An before study reported an even higher percentage of PE patients with normal D-dimer values—26% (42). Whereas other studies, in agreement with our results, reported that iii.4% of 382 patients (43), 3.6% of 55 patients (44), and 4% of 725 patients (45) with PE had normal plasma D-dimer values, which is compatible with our results. Another study has shown that 2 of 5 (40%) patients with normal with plasma D-dimer levels had PE or DVT (46). These results are comparable with our results, where 3 of vii (42.8%) patients with plasma D-dimer levels <500 ng/mL had acute PE. Some other study too encourages physicians to search for astute PE in patients with normal D-dimer values, when symptoms can't be explained otherwise (can't be connected with another affliction), in the presence of thromboembolism risk factors and when duration of symptoms is unnaturally long (45). We also considered what could explain negative D-dimer results on those patients. Most often false-negative results are caused by anticoagulation therapy (47)—all patients in our study were hospitalized so they could use antithrombotic prophylaxis and 3 of them were already treated because of DVT or stroke before PE diagnosis.
The 2014 European Social club of Cardiology (ESC) guidelines on the diagnosis and management of astute PE state that a normal plasma D-dimer level renders acute PE or DVT unlikely just also that the quantitative latex-derived assays (used in our study) and a whole-claret agglutination assay have a diagnostic sensitivity <95% and are thus oftentimes referred to equally moderately sensitive. In outcome studies, those assays proved to be rubber in ruling out PE in PE—unlikely patients as well equally in patients with a low clinical probability. Their safe in ruling out PE has not been established in the intermediate clinical probability category (36). Our study in combination with previously cited studies (42,43,45,46) confirm results the guidelines, however nosotros suggest, that clinicians should also include information about patients with normal plasma D-dimer level, especially if had previous PE or DVT, elapsing of symptoms is unnaturally long or when symptoms tin can't exist explained otherwise.
Our study was based on the retrospective analysis of the medical notes of patients in a hospital database, which prevented united states of america from checking reasons for ordering the plasma D-dimer exam and the time frame from symptoms to CTPA. We besides did non include cases in which PE was diagnosed without previous D-dimer tests and patients who were diagnosed with acute PE without using CTPA, because contraindicated. However, these cases were few, and information technology is unlikely that they would have changed the results of our written report. Unfortunately, because of the retrospective blueprint of our study we did non have the possibility to apply the Geneva score or modified Wells criteria and not always the score of these scales was recorded in the medical notes of our patients, despite the 2014 ESC Guidelines on the diagnosis and management of acute PE recommend to assess the clinical probability of acute PE diagnosis (36). The value of this clinical evaluation has been confirmed in few clinical studies for example the prospective investigation on PE diagnosis (PIOPED) (48). The small number of patients included in our study does not allow to depict clear conclusions almost utility hazard factors like cancer, pregnancy or post-surgery to obtain dissimilar plasma D-dimer cut-off values for those patients and prospective studies in this area are needed.
Conclusions
In general population of patients with plasma D-dimer levels exceeding at to the lowest degree iv times (in our study 2,152 ng/mL) its normal value, CTPA should be considered predictive even for patients with a low clinical probability of astute PE. However, the small number of patients included in our report does not allow united states of america to describe articulate conclusions nearly patients with cancer, pregnancy or post-surgery that are also often associated with increased plasma D-dimer levels. Besides, the age >65 years and a history of neoplasm, should always be considered in suspecting acute PE, considering may significantly increase the plasma D-dimer cutting-off level associated with an increased likelihood of acute PE.
Acknowledgements
Funding: This piece of work is supported by Medical University of Silesia (grant number KNW-i-052/N/7/G).
Conflicts of Interest: The authors have no conflicts of involvement to declare.
Ethical Statement: The research was conducted according to the principles of the Declaration of Helsinki. And in Poland (according to the smoothen law) studies which are non experimental—including retrospective analyses or observational studies—do not require upstanding committee blessing.
References
- Goldhaber SZ. Venous thromboembolism: epidemiology and magnitude of the problem. Best Pract Res Clin Haematol 2012;25:235-42. [Crossref] [PubMed]
- Bronić A. Thromboembolic diseases as biological and clinical syndrome—office of the mediterranean league against thromboembolic diseases. Biochem Med 2010;twenty:ix-12. [Crossref]
- Heit JA. The epidemiology of venous thromboembolism in the community. Arterioscler. Thromb. Vasc. Biol 2008;28:370-ii. [Crossref] [PubMed]
- Gupta RT, Kakarla RK, Kirshenbaum KJ, et al. D-Dimers and efficacy of clinical run a risk interpretation algorithms: sensitivity in evaluation of astute pulmonary embolism. AJR Am J Roentgenol 2009;193:425-thirty. [Crossref] [PubMed]
- Zhu T, Martinez I, Emmerich J. Venous thromboembolism: take a chance factors for recurrence. Arterioscler Thromb Vasc Biol 2009;29:298-310. [Crossref] [PubMed]
- Bĕlohlávek J, Dytrych Five, Linhart A. Pulmonary embolism, function I: epidemiology, risk factors and run a risk stratification, pathophysiology, clinical presentation, diagnosis and nonthrombotic pulmonary embolism. Exp Clin Cardiol 2013;18:129-38. [PubMed]
- Lloyd-Jones D, Adams RJ, Brown TM, et al. Executive summary: centre disease and stroke statistics--2010 update: a report from the American Heart Clan. Circulation 2010;121:948-54. [Crossref] [PubMed]
- Liu CP, Li XM, Chen HW, et al. Depression, anxiety and influencing factors in patients with acute pulmonary embolism. Mentum Med J (Engl) 2011;124:2438-42. [PubMed]
- Conget F, Otero R, Jimenez D, et al. Short-term clinical consequence after acute symptomatic pulmonary embolism. Thromb Haemost 2008;100:937-42. [Crossref] [PubMed]
- den Exter PL, van der Hulle T, Lankeit M, et al. Long-term clinical grade of astute pulmonary embolism. Claret Rev 2013;27:185-92. [Crossref] [PubMed]
- Cohen AT, Agnelli 1000, Anderson FA, et al. Venous thromboembolism (VTE) in Europe—the number of VTE events and associated morbidity and mortality. Thromb Haemost 2007;98:756-64. [Crossref] [PubMed]
- Konstantinides SV. 2014 ESC Guidelines on the diagnosis and management of astute pulmonary embolism. Eur Middle J 2014;35:3145-6. [PubMed]
- Greenish SM, Yealy DM. Correct-Sizing testing for pulmonary embolism: recognizing the risks of detecting any jell. Ann Emerg Med 2012;59:524-half dozen. [Crossref] [PubMed]
- Gaffney PJ, Creighton LJ, Callus M, et al. Monoclonal antibodies to crosslinked fibrin deposition products (XLFDP). two. evaluation in a multifariousness of clinical atmospheric condition. Br J Haematol 1988;68:91-half-dozen. [Crossref] [PubMed]
- Bounameaux H, Slosman D, Demoerloose P, et al. Diagnostic value of plasma d-dimer in suspected pulmonary embolism. Lancet 1988;2:628-9. [Crossref] [PubMed]
- Plasma d-dimer and pulmonary embolism. Lancet 1989;1:791-2. [PubMed]
- Bounameaux H, Cirafici P, Demoerloose P, et al. Measurement of d-dimer in plasma every bit diagnostic aid in suspected pulmonary embolism. Lancet 1991;337:196-200. [Crossref] [PubMed]
- Ginsberg JS, Wells PS, Brilledwards P, et al. Application of a novel and rapid whole claret assay for didimer in patients with clinically suspected pulmonary embolism. Thromb Haemost 1995;73:35-8. [Crossref] [PubMed]
- Perrier A, Bounameaux H, Morabia A, et al. Diagnosis of pulmonary embolism past a decision analysis-based strategy including clinical probability, D-dimer levels, and ultrasonography: a management written report. Arch Intern Med 1996;156:531-vi. [Crossref] [PubMed]
- Perrier A, Desmarais Due south, Goehring C, et al. D-dimer testing for suspected pulmonary embolism in outpatients. Am J Respir Crit Care Med 1997;156:492-6. [Crossref] [PubMed]
- Ginsberg JS, Wells PS, Kearon C, et al. Sensitivity and specificity of a rapid whole-claret analysis for D-dimer in the diagnosis of pulmonary embolism. Ann Intern Med 1998;129:1006. [Crossref] [PubMed]
- Wells PS, Anderson DR, Rodger M, et al. Derivation of a simple clinical model to categorize patients probability of pulmonary embolism: increasing the models utility with the SimpliRED D-dimer. Thromb Haemost 2000;83:416-xx. [Crossref] [PubMed]
- Wells PS, Anderson DR, Rodger Chiliad, et al. Excluding pulmonary embolism at the bedside without diagnostic imaging: management of patients with suspected pulmonary embolism presenting to the emergency department past using a simple clinical model and D-dimer. Ann Intern Med 2001;135:98-107. [Crossref] [PubMed]
- Kruip MJ, Slob MJ, Schijen JH, et al. Use of a clinical decision rule in combination with D-dimer concentration in diagnostic workup of patients with suspected pulmonary embolism—a prospective management written report. Arch Intern Med 2002;162:1631-5. [Crossref] [PubMed]
- 10 Wolde G, Hagen PJ, Macgillavry MR, et al. Non-invasive diagnostic piece of work-up of patients with clinically suspected pulmonary embolism; results of a direction written report. J Thromb Haemost 2004;two:1110-7. [Crossref] [PubMed]
- van Belle A, Buller Hour, Huisman MV, et al. Effectiveness of managing suspected pulmonary embolism using an algorithm combining clinical probability, D-dimer testing, and computed tomography. JAMA 2006;295:172-ix. [Crossref] [PubMed]
- Becattini C, Lignani A, Masotti L, et al. D-Dimer for gamble stratification in patients with acute pulmonary embolism. J Thromb Thrombolysis 2012;33:48-57. [Crossref] [PubMed]
- Ghanima W, Abdelnoor M, Holmen LO, et al. D-dimer level is associated with the extent of pulmonary embolism. Thromb Res 2007;120:281-8. [Crossref] [PubMed]
- Verhovsek One thousand, Douketis JD, Yi Q, et al. Systematic review: D-dimer to predict recurrent illness later on stopping anticoagulant therapy for unprovoked venous thromboembolism. Ann Intern Med 2008;149: 481-ninety, W94.
- Ji Y, Dominicus B, Juggessur-Mungur KS, et al. Correlation of D-dimer level with the radiological severity indexes of pulmonary embolism on computed tomography pulmonary angiography. Mentum Med J (Engl) 2014;127:2025-9. [PubMed]
- Shah K, Quaas J, Rolston D, et al. Magnitude of D-dimer matters for diagnosing pulmonary embolus. Am J Emerg Med 2013;31:942-5. [Crossref] [PubMed]
- Tick LW, Nijkeuter M, Kramer MHH, et al. High D-dimer levels increase the likelihood of pulmonary embolism. J Intern Med 2008;264:195-200. [Crossref] [PubMed]
- Legnani C, Cini K, Scarvelis D, et al. Multicenter evaluation of a new quantitative highly sensitive D-dimer assay, the Hemosil D-dimer HS 500, in patients with clinically suspected venous thromboembolism. Thromb Res 2010;125:398-401. [Crossref] [PubMed]
- Arnautović-Torlak V, Pojskić B, Zutic H, et al. Values of D-dimer test in the diagnostics of pulmonary embolism. Med Glas (Zenica) 2014;11:258-63. [PubMed]
- Di Nisio Thou, Squizzato A, Rutjes AW, et al. Diagnostic accurateness of D-dimer exam for exclusion of venous thromboembolism: a systematic review. J Thromb Haemost 2007;5:296-304. [Crossref] [PubMed]
- Konstantinides SV, Torbicki A, Agnelli K, et al. 2014 ESC Guidelines on the diagnosis and management of acute pulmonary embolism: the job force for the diagnosis and management of astute pulmonary embolism of the european club of cardiology (ESC). Eur Heart J 2014;35:3033-69, 3069a-1000.
- Raimondi P, Bongard O, Demoerloose P, et al. D-dimer plasma concentration in various clinical atmospheric condition—implication for the use of this exam in diagnostic arroyo of venous thromboembolism. Thromb Res 1993;69:125-30. [Crossref] [PubMed]
- Righini K, Van Es J, Den Exter PL, et al. Age-adjusted D-dimer cutoff levels to rule out pulmonary embolism: the ADJUST-PE study. JAMA 2014;311:1117-24. [Crossref] [PubMed]
- Wilts IT, Le Gal G, den Exter PL, et al. PO-29—historic period-adjusted D-dimer cutoff level increases the number of cancer patients in who pulmonary embolism tin can be safely excluded without CT-PA imaging: the ADJUST-PE cancer substudy. Thromb Res 2016;140 Suppl 1:S187. [Crossref] [PubMed]
- Le Gal Thousand, Righini M, Roy PM, et al. Prediction of pulmonary embolism in the emergency department: the revised Geneva score. Ann Intern Med 2006;144:165-71. [Crossref] [PubMed]
- Karamat A, Awan Southward, Hussain MG, et al. Usefulness of clinical prediction rules, D-dimer, and arterial claret gas analysis to predict pulmonary embolism in cancer patients. Oman Med J 2017;32:148-53. [Crossref] [PubMed]
- Kutinsky I, Blakley Due south, Roche 5. Normal D-dimer levels in patients with pulmonary embolism. Arch Intern Med 1999;159:1569-72. [Crossref] [PubMed]
- Gibson NS, Sohne M, Gerdes VEA, et al. The importance of clinical probability assessment in interpreting a normal d-dimer in patients with suspected pulmonary embolism. Breast 2008;134:789-93. [Crossref] [PubMed]
- Dunn KL, Wolf JP, Dorfman DM, et al. Normal D-dimer levels in emergency section patients suspected of acute pulmonary embolism. J Am Coll Cardiol 2002;40:1475-8. [Crossref] [PubMed]
- Guo Z, Ma Q, Zheng Y, et al. Normal blood D-dimer concentrations: practise they exclude pulmonary embolism? Mentum Med J (Engl) 2014;127:eighteen-22. [PubMed]
- Parent F, Maitre S, Meyer 1000, et al. Diagnostic value of D-dimer in patients with suspected pulmonary embolism: results from a multicentre outcome study. Thromb Res 2007;120:195-200. [Crossref] [PubMed]
- Couturaud F, Kearon C, Bates SM, et al. Subtract in sensitivity of D-dimer for acute venous thromboembolism later on starting anticoagulant therapy. Claret Coagul Fibrinolysis 2002;13:241-6. [Crossref] [PubMed]
- Stein PD, Woodard PK, Weg JG, et al. Diagnostic pathways in acute pulmonary embolism: recommendations of the PIOPED Ii investigators. Am J Med 2006;119:1048-55. [Crossref] [PubMed]
Cite this commodity as: Sikora-Skrabaka Chiliad, Skrabaka D, Ruggeri P, Caramori G, Skoczyński Southward, Barczyk A. D-dimer value in the diagnosis of pulmonary embolism—may it exclude only? J Thorac Dis 2019;eleven(3):664-672. doi: 10.21037/jtd.2019.02.88
bradfordsplad1968.blogspot.com
Source: https://jtd.amegroups.com/article/view/27615/html
0 Response to "Rapid Systematic Review Age-adjusted D-dimer for Ruling Out Pulmonary Embolism"
Post a Comment